…Looming Crisis in the Face of Inadequate Health Care
Lerato Matheka and Marcia Zali
“Go talk to your mother; she is dying.” These are the words that changed Molulela Ntee’s life, as she recalls the day an oncologist at Universitas Hospital in Bloemfontein, South Africa, told her the devastating news about her mother’s condition.
After two years of watching her mother’s health deteriorate, nothing could have prepared her for the bleak future that lay ahead, a future without her dear mother.
“It was confusing, I couldn’t understand the gravity of the situation. My mind refused to accept the harsh reality unfolding before me,” Molulela recalls, her voice quivering with emotion.
“I remember giving the doctor a weak smile, dismissing his words as mere conjecture. In my heart, I believed that the nurses were doing everything they could to save her, that she would pull through and go back to her old self, healthy and happy,” she recounts.
Molulela’s tale is not just one of personal tragedy, but a damning indictment of the glaring inadequacies that plague Lesotho’s healthcare system—a system riddled with shortcomings and negligence that have cost countless lives and shattered families.
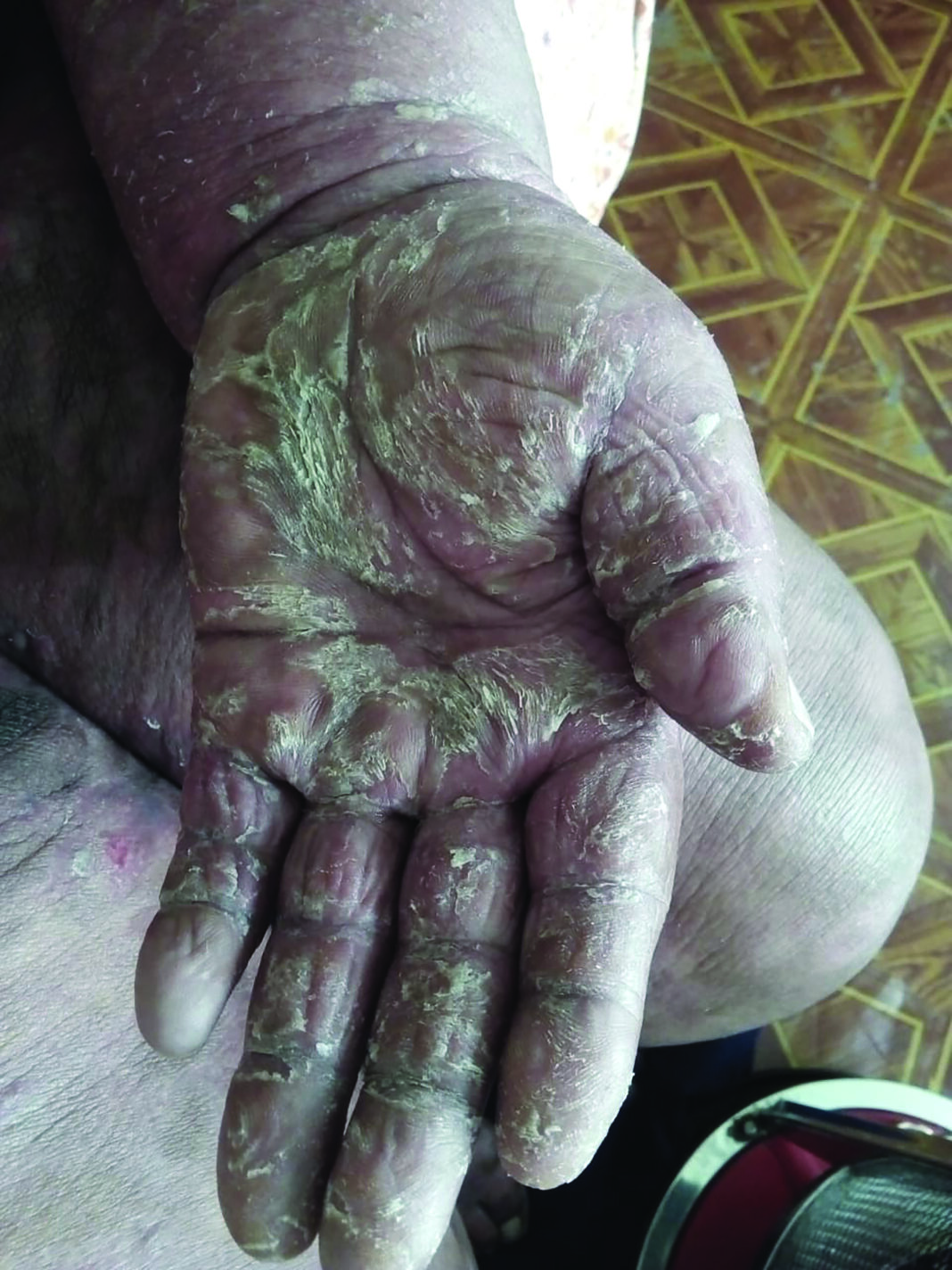
Their journey began in 2016, with a seemingly benign ringworm-like illness that soon spiralled into a nightmare of suffering. As time went on, the unknown illness refused to heal, resulting in an unending cycle of suffering that could not be diagnosed or treated successfully.
From private clinics to the overcrowded wards of government hospitals, Molulela and her mother sought answers, only to be met with indifference and incompetence at every turn.
“It felt like we were drowning in a sea of incompetence. Doctors shuffled us from one diagnosis to another—Alzheimer’s, psoriasis, each more baffling than the last. Yet, during the confusion, one thing remained constant: my mother’s suffering knew no end.”
As her mother’s health deteriorated, Molulela found herself fighting against a healthcare system that seemed determined to cast her aside.
The doctors could not understand the severity of her mother’s illness.
“I can never forget that morning, 12 March 2018. The doctors discussed giving my mother a ‘merciful killing.’ I took them on and demanded that my mother be admitted so the hospital could ease her pain.”
Admitted for a week, there seemed to be hope. Tests were run and she looked better until she was sent back home.
Shortly after she was discharged, she experienced some swelling on her body.
“When we returned, she was worse than before but they refused to admit her or even to attempt helping me. All they did was give her an injection to help with the swelling. The hospital wasn’t going to help me,” she recounts, saying the journey left her financially dry.
“I then remembered that patients are treated in Bloemfontein and I demanded to have my mother transferred to South Africa, but it was too late,” she says, noting it was not until her mother was admitted to Universitas Hospital in Bloemfontein that the truth was finally revealed—a devastating diagnosis of skin cancer, lymphoma, a cruel twist of fate that robbed them of any hope of a future together.
“She initially had skin cancer which later developed into lymphoma. Her death could have been prevented if not for the years of misdiagnosis and neglect.”
But Molulela’s story is not just one of loss—it is a call to action, a rallying cry for change in a system that has failed its people several times.
As Molulela navigates the journey of healing, she boldly confronts a health system she describes as “riddled with shortcomings and negligence—a system that failed her mother, and countless others like her.
“Our healthcare system is broken. It is a system that values bureaucracy over compassion, and indifference over empathy. Until we demand change and hold our leaders accountable, more lives will be lost, more families will be torn apart,” she asserts.
The fate of misdiagnosis is one faced by many Basotho patients, coupled with other interlinked weak systems, and for Limakatso*, what began as a mere abdominal pain soon spiralled into a nightmare of misdiagnoses and unanswered questions.
“I was told it was just hormonal imbalances and I learned to make peace with the disease. I was prepared to endure the pain without hope of a proper diagnosis.” she says.
With each visit to the clinic, she was met with the same routine: different medications, fleeting moments of relief, and the hollow promise of a return to normalcy.
But, the pain continued, accompanied by swelling and discomfort, symptoms that no one could explain the cause behind them. The unbearable pain led to her determination to find answers, refusing to accept the status quo any longer.
“I was fortunate to encounter a doctor who listened, who questioned the prevailing narrative. He ordered a pelvic ultrasound scan, suspecting there was more to my condition than meets the eye.”
The results of the scan revealed a truth she had long feared: an ovarian mass, a silent danger lurking within her body.
While she was terrified by the discovery, it brought her some clarity and hope that she would get healed.
Blood currency for surgery
Yet, even as she faced the daunting prospect of surgery, she found herself confronted with yet another obstacle: the dire shortage of blood in the country.
“I was told I needed to produce three pints of blood as ‘currency’ for my surgery. It was a cruel twist of fate, a reminder of the fragility of life in the face of bureaucratic indifference,” she recalls, her voice tinged with disbelief.
With no one to turn to, she took to social media, pleading for assistance from friends and strangers alike.
“It was a race against time because, without proof of donation, my next appointment was going to be a year away, the time I didn’t think I had, but thanks to the kindness of others, the currency came through and I was able to undergo surgery and take the first step towards healing.”
The results of the surgery brought mixed emotions as they confirmed that the tumour was cancerous, described as an ovarian cancer.
As she awaits the results of further tests in Bloemfontein, she remains steadfast in her determination to overcome the odds, to emerge from the shadows of her past stronger and more resilient than ever before.
“This journey has taught me the importance of speaking out against injustice, and as I look forward to a new chapter in my life, I vow to be a voice for those who have been silenced by the failings of our healthcare system.”
Cancer Burden in Lesotho: A Harrowing Reality
Lesotho’s only Clinical Radiation Oncologist, Dr Kabelo Mputsoe, pointed out that cervical cancer is the most common cancer affecting women and the most common cause of cancer deaths in Lesotho.
According to Mputsoe, cervical cancer if found in the early stages is curable with radiotherapy.
Mputsoe explained that more than 40 percent of women are diagnosed at the late stage of cervical cancer and thus rarely recover.
She noted that between June 2020 and August 2022, Lesotho has 12 types of cancers registered at Senkatana Cancer Clinic. Cervical cancer tops the list with 560 cases followed by breast cancer with 170 cases. Prostate cancer came third with 136 cases followed by endometrial cancer with 24 cases and lung cancer with 19 cases.
Mputsoe further stated that demographic characteristics of cancer patients have also shown that for 2022 there were 531 cases where females made up to 396 (81 percent) and males 19 percent with 92 cases.
Overall cases for 2023, the doctor said Lesotho recorded 604 cases, 466 females (77.2 percent” and men with 138 cases (22.8 percent).
“In terms of age groups most of the cancer cases are found in elderly people who are 50 and above.”
Cancer burden in South Africa
While cancer patients from Lesotho are transported to South Africa for treatment, South Africa is facing obstacles of its own, with an overburdened healthcare system that is faced with numerous challenges.
According to Statistics South Africa, over 85 300 cancer cases were diagnosed in 2019 and out of those, over 43 811 (51.3 percent) were women while 41 491 (48.6 percent) were men.
Breast cancer was the most diagnosed cancer amongst women with 10 172 (23.2 percent) followed by cervical cancer, colorectal cancer, skin cancer and uterus cancer. For men, the mostly diagnosed cancer was prostate cancer with 10 495 (25.3 percent). It was then followed by different types of skin cancer, colorectal cancer, lung cancer and non-Hodgkin’s lymphoma (cancer in the lymphatic system).
The Cancer Alliance, an advocacy group for cancer patients, reports that the availability and access to cancer treatment in South Africa is highly dependent on one’s ability to afford private healthcare. This is because the majority of patients (86 percent) rely on public health that only has 20 percent of the oncology staff. In contrast to this, the 14 percent of the population that can afford private healthcare have access to 80 percent oncologist staff.
A gap that has seen patients in the public healthcare sector waiting up to 6 months before they are seen by a specialist while others have been on the waiting list for years.
“There is a severe under-resourcing, not only of staff, but also of equipment. And also when we start talking about the budget for chemotherapy, budgets within the various provinces are not enough to treat cancer patients,” said the chairperson of the Cancer Alliance, Salome Meyer.
Despite these challenges, Meyer added that where services are available and delivered, lives are saved – yet, more can be done to improve access to care, especially from the primary healthcare level where most delays in the detection of cancer sooner occur.
Sharing Meyer’s sentiment, CEO of Campaigning for Cancer, Lauren Pretorius said that the state of oncology diagnostic and treatment services are good for some cancer types, like breast cancer, but dismal for others, like prostate cancer. This was mainly because of the poor implementation of policies that are meant to improve cancer treatment and the disinvestment in palliative care by donors and the government.
“There is an increasing concern about the equity problem, specifically regarding the accessibility of specialist treatment and care. At rural public facilities, patients do not receive accurate screening, early detection, and appropriate treatment.
According to Pretorius, the lack of access to treatment for cancer patients was a failure of the healthcare system that sees patients making several trips to underequipped and understaffed facilities until they eventually die even in instances where they could be saved.
Meyer on the other hand believes that South Africa’s challenges go beyond trying to assist patients from Lesotho to access cancer treatment because patients from other countries in the Southern Africa Development Community (SADC) also seek the services from South Africa.
“Another problem that we’re ignoring is that migrant workers that have been in this country for a number of years, who are now diagnosed with cancer, are not going to get any treatment because they are undocumented,” she added.
It is because of these challenges that Meyer believes that there should be a regional effort to address the cancer burden and avoid overburdening an already overburdened healthcare system.
Lesotho’s Medical Debt Crisis: A Looming Disaster
Minister of Health Selibe Mochoboroane has decried the high cost of treating cancer patients in South Africa.
“Between 2015 and 2016, we used to spend between about M114,000 and M140,000 to treat one cancer patient in Bloemfontein,” Mochoborane revealed.
“From 2022 to date, we are spending about M220,000 to treat one cancer patient,” he added.
The minister said many people were dying of cancer because of several reasons. In 2022 alone, over 600 new cases of cancer were recorded across the country.
Lesotho is grappling with a significant medical debt amounting to M211 million owed to the Free State government in South Africa for healthcare services.
This staggering debt has accumulated over the years, as revealed in the consolidated report on the annual budget and estimates of revenue and expenditure for the financial year 2024/2025.
Presented by the portfolio committee on the Economic and Development Cluster to the National Assembly of Lesotho on March 8, 2024, the report also highlights an additional unbudgeted M108 million intended to cover Queen ‘Mamohato Memorial Hospital referrals to South Africa for the upcoming fiscal year.
Health Minister Selibe Mochoboroane, in an exclusive interview with Newsday, confirmed the country’s indebtedness to South Africa, emphasising its longstanding nature and the challenges posed by unpaid arrears.
“The debt has been accumulated over many years and is being bloated by unpaid arrears,” he said.
Mochoboroane further revealed the disproportionate burden borne by cancer patients, with the country spending over M200 million monthly on referrals to South Africa.
Lesotho’s commitment
In response to the escalating costs of referrals, the committee underscored the urgency of constructing a Cancer Treatment and Management Centre.
Mochoboroane also acknowledged delays in this regard but assured progress.
“The first phase of the project has started and is almost 80% complete, with the second phase, involving tender evaluations, currently underway,” he stated.
He emphasised the potential cost-saving benefits once the facility becomes operational.
“Once completed, the Cancer facility will save the country M200 million annually,” he said.
Addressing the funding shortfall, the committee recommended transferring M250 million from the Lesotho Millennium Development Account (LMDA) to the health ministry. However, Mochoboroane admitted the absence of a concrete payment strategy for the medical debt, citing years of neglect in servicing the loan.
He warned of potential repercussions, including the refusal of future patients by South Africa if the debt remains unresolved.
“If the country doesn’t service its debt Lesotho may be going towards a point where South Africa will no longer take patients from Lesotho,” he said, however, was quick to indicate his ministry was working tirelessly to prevent such a scenario.
Despite these challenges, Mochoboroane expressed optimism about the country’s healthcare future, underpinned by ongoing reforms aimed at enhancing service delivery and financial sustainability.
“We are in a dire situation, but with the government’s commitment, we will overcome,” he asserted.
In light of these developments, the government is faced with a critical juncture, poised between the urgent need for fiscal prudence and the imperative of ensuring access to life-saving healthcare services.
As Lesotho grapples with its medical debt crisis, the plight of its citizens hangs in the balance, a stark reminder of the human cost of bureaucratic negligence and fiscal mismanagement.
Officials from both the provincial and national health departments in South Africa had not responded to questions at the time of printing


Summary
- ” These are the words that changed Molulela Ntee’s life, as she recalls the day an oncologist at Universitas Hospital in Bloemfontein, South Africa, told her the devastating news about her mother’s condition.
- In my heart, I believed that the nurses were doing everything they could to save her, that she would pull through and go back to her old self, healthy and happy,” she recounts.
- “I then remembered that patients are treated in Bloemfontein and I demanded to have my mother transferred to South Africa, but it was too late,” she says, noting it was not until her mother was admitted to Universitas Hospital in Bloemfontein that the truth was finally revealed—a devastating diagnosis of skin cancer, lymphoma, a cruel twist of fate that robbed them of any hope of a future together.

Your Trusted Source for News and Insights in Lesotho!
At Newsday Media, we are passionate about delivering accurate, timely, and engaging news and multimedia content to our diverse audience. Founded with the vision of revolutionizing the media landscape in Lesotho, we have grown into a leading hybrid media company that blends traditional journalism with innovative digital platforms.